Streptococcus: A Comprehensive Overview of the Bacterium and Its Clinical Implications
Introduction
Streptococcus is a genus of Gram-positive, non-motile, non-spore-forming, catalase-negative cocci that typically grow in chains or pairs. These bacteria are facultative anaerobes and are characterized by their ability to cause a wide spectrum of diseases ranging from mild skin infections to life-threatening invasive diseases. The genus comprises numerous species with varying degrees of pathogenicity, with Streptococcus pyogenes (Group A Streptococcus) and Streptococcus pneumoniae being among the most clinically significant.
Classification and Identification
Streptococci are traditionally classified based on their hemolytic properties on blood agar:
- Alpha-hemolytic: Partial hemolysis with a greenish discoloration around colonies
- Beta-hemolytic: Complete hemolysis with clear zones around colonies
- Gamma-hemolytic: No hemolysis
Additionally, beta-hemolytic streptococci are further categorized using the Lancefield grouping system (Groups A through V) based on cell wall carbohydrate antigens. Modern identification methods include MALDI-TOF mass spectrometry and molecular techniques such as 16S rRNA gene sequencing, which have significantly improved accurate species identification.
Major Pathogenic Species and Associated Infections
Streptococcus pyogenes (Group A Streptococcus)
S. pyogenes is responsible for a variety of suppurative and non-suppurative sequelae:
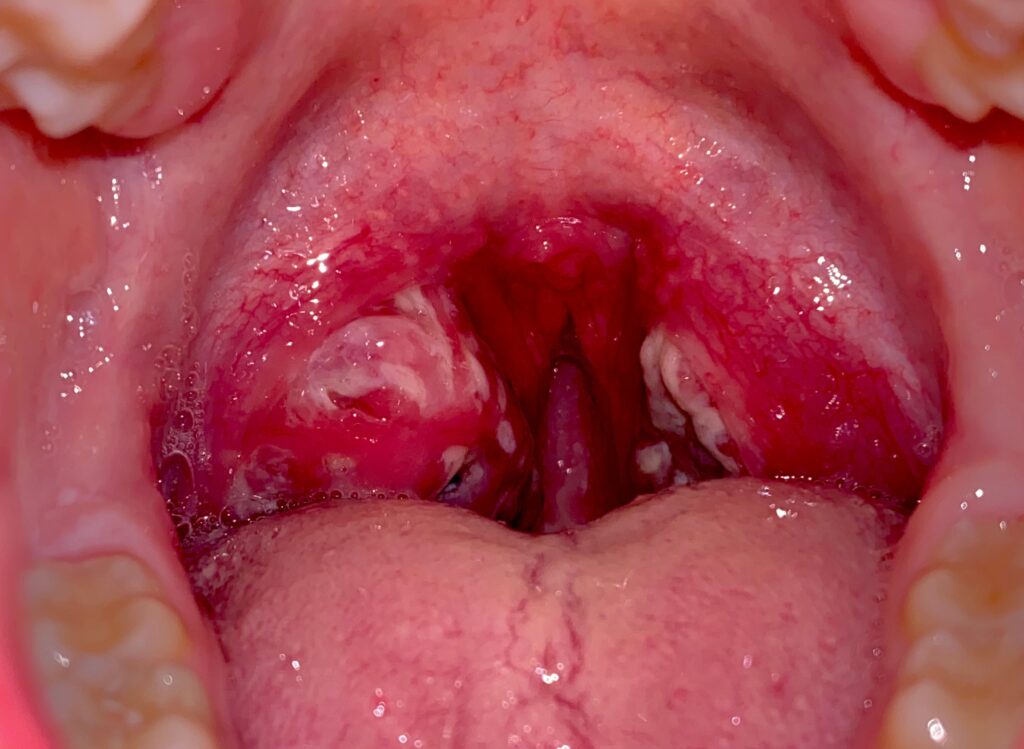
- Pharyngitis/Tonsillitis: “Strep throat” accounts for 15-30% of pediatric sore throats and 5-10% in adults. Recent studies have shown increasing antibiotic resistance patterns, particularly in certain geographic regions.
- Skin and Soft Tissue Infections:
- Impetigo: Superficial skin infection primarily affecting children
- Erysipelas: Infection of the upper dermis and superficial lymphatics
- Cellulitis: Infection of the deeper dermis and subcutaneous fat
- Necrotizing fasciitis: Rapidly progressing infection of the fascial planes, with mortality rates still exceeding 20% despite advances in treatment
- Post-streptococcal Sequelae:
- Acute rheumatic fever (ARF): Inflammatory disease affecting the heart, joints, skin, and brain
- Post-streptococcal glomerulonephritis: Immune complex-mediated kidney disease
- Streptococcal Toxic Shock Syndrome (STSS): Severe systemic illness characterized by hypotension, multi-organ failure, and high mortality rates (30-70%).
Streptococcus pneumoniae
S. pneumoniae remains a leading cause of morbidity and mortality worldwide despite vaccination efforts:
- Pneumonia: Community-acquired pneumonia remains the most common serious manifestation, with S. pneumoniae responsible for approximately 25% of all cases.
- Otitis Media: A common infection in children, with S. pneumoniae isolated in 30-40% of cases.
- Sinusitis: Accounts for 20-43% of bacterial sinusitis cases.
- Meningitis: Though vaccination has reduced incidence, S. pneumoniae remains a leading cause of bacterial meningitis with mortality rates of 15-30%.
- Bacteremia: Invasive pneumococcal disease carries significant mortality, particularly in elderly and immunocompromised individuals.
Streptococcus agalactiae (Group B Streptococcus)
GBS is particularly significant in maternal and neonatal medicine:
- Neonatal Infections:
- Early-onset disease (within 7 days of birth): Presenting as sepsis, pneumonia, or meningitis
- Late-onset disease (7-90 days): Typically presenting as meningitis or bacteremia
- Maternal Infections:
- Urinary tract infections
- Chorioamnionitis
- Endometritis
- Bacteremia
- Infections in Non-pregnant Adults:
- Skin and soft tissue infections
- Bacteremia
- Pneumonia
- Bone and joint infections
Viridans Group Streptococci
This diverse group includes S. mutans, S. mitis, S. salivarius, and others:
- Dental Caries: S. mutans is a primary causative agent in dental decay.
- Infective Endocarditis: Viridans streptococci are leading causes of native valve endocarditis, accounting for 30-40% of cases.
- Bacteremia: Particularly in immunocompromised hosts and following dental procedures.
Streptococcus anginosus Group (S. anginosus, S. intermedius, S. constellatus)
This group has a propensity for abscess formation:
- Deep-tissue Abscesses:
- Brain abscesses
- Liver abscesses
- Lung abscesses
- Intra-abdominal abscesses
- Empyema: Purulent infection of the pleural space.
Emerging Concerns and Recent Developments
Antimicrobial Resistance
Recent surveillance data from 2022-2023 indicate concerning trends in antimicrobial resistance:
- Macrolide Resistance: Increasing macrolide resistance in S. pyogenes has been reported globally, with rates exceeding 20% in some regions.
- Penicillin Non-susceptibility: While S. pyogenes remains universally susceptible to penicillin, reduced susceptibility to penicillin in S. pneumoniae continues to be a concern, particularly in Asia and parts of Europe.
- Multidrug Resistance: The emergence of multidrug-resistant strains of S. pneumoniae poses significant therapeutic challenges.
Hypervirulent Strains
Recent molecular epidemiological studies have identified emergence of hypervirulent strains of GAS, particularly those associated with the resurgence of scarlet fever and invasive disease in different parts of the world. Genomic analyses have revealed horizontal gene transfer events contributing to increased virulence.
Vaccine Development
The pneumococcal conjugate vaccine (PCV13) and the newer 20-valent pneumococcal conjugate vaccine (PCV20) have significantly reduced the burden of invasive pneumococcal disease. However, serotype replacement remains a challenge. Development of GBS vaccines has progressed to clinical trials, with promising results for maternal immunization strategies to prevent neonatal disease.
Diagnosis and Management
Rapid molecular diagnostic tests have revolutionized the identification of streptococcal infections, allowing for faster and more accurate diagnosis. Point-of-care testing for GAS pharyngitis has improved diagnostic accuracy and reduced unnecessary antibiotic use.
Treatment typically involves:
- Beta-lactam antibiotics (penicillins, cephalosporins) remain the first-line therapy for most streptococcal infections
- Macrolides or clindamycin for patients with penicillin allergy
- Vancomycin or newer agents like linezolid, daptomycin, or ceftaroline for resistant strains
- Surgical intervention for abscesses and necrotizing infections
Conclusion
Streptococcal infections continue to pose significant clinical challenges despite advances in diagnosis, treatment, and prevention. The emergence of antimicrobial resistance and hypervirulent strains underscores the importance of ongoing surveillance, judicious antibiotic use, and continued vaccine development. Understanding the diverse manifestations of streptococcal infections is essential for prompt recognition and appropriate management to reduce associated morbidity and mortality.
References:
- Vekemans J, Crofts J, Baker CJ, et al. (2023). “A roadmap for Group B Streptococcus vaccine development: Expert consensus and priority pathways for early-phase clinical trials.” Vaccine, 41(1):10-18.
- Furfaro LL, Chang BJ, Payne MS. (2022). “Perinatal Streptococcus agalactiae (Group B Streptococcus) epidemiology and vaccines: Current status and future priorities.” Frontiers in Microbiology, 13:1034790.
- Whittaker E, Bamford A, Riley P, et al. (2022). “Streptococcal infections in the paediatric population—when to worry and when to refer.” British Journal of General Practice, 72(716):133-134.
- Brouwer S, Raeven VM, van den Dobbelsteen GP, et al. (2023). “Group A Streptococcus: A persistent threat and promising vaccine target.” NPJ Vaccines, 8(1):67.
- Loughran AJ, Turner RE, Peng Z, et al. (2023). “Type I-E CRISPR-Cas systems shape Group A Streptococcus genetic diversity and pathogenesis.” Nature Communications, 14(1):1294.
- Leung MH, Bryson KM, Freystatter K, et al. (2022). “Increasing invasive Group A Streptococcal disease in Australia, 2014-2019: bacteriological and epidemiological findings from the Australian Group A Streptococcal surveillance programme.” The Lancet Regional Health – Western Pacific, 28:100550.
- Bessen DE, Smeesters PR, Beall BW. (2022). “Molecular epidemiology, ecology, and evolution of group A streptococci.” Microbiology Spectrum, 10(1)
.
- Chochua S, Metcalf BJ, Li Z, et al. (2022). “Population and genomic analysis of phenotypically penicillin-resistant group A Streptococcus.” Journal of Clinical Microbiology, 60(6)
.
- de Steenhuijsen Piters WAA, Jochems SP, Mitsi E, et al. (2023). “Streptococcus pneumoniae colonization and the nasopharyngeal microbiome: host-microbe interactions and regulation of invasive disease.” Microbiome, 11(1):23.
- Lamagni T, Guy R, Chand M, et al. (2023). “Resurgence of scarlet fever and invasive group A streptococcal infections in the UK, 2014–2022: population-based surveillance study.” The Lancet Infectious Diseases, 23(9):1061-1071.

Nancy L. Kimmel obtained her PhD in Environmental Engineering in 2002, then went on to teach Physics and Mechanical Engineering at Lawrence Technological University, Henry Ford College and Oakland University. She obtained her Associate in Nursing from Henry Ford College and then went on to earn her Master Degree as a Family Nurse Practitioner and became Board Certified working as a licensed FNP in the State of Michigan. She then went on to Medical School where she is now in her 3rd year, and is also in the process of obtaining her Doctorate in Nursing Practice through Chamberlin University. She has authored the NET Study Guide, as well a several books on subjects of Math, ECG/EKG and Phlebotomy. She holds a patent on an Air Filter through the U.S. Patent Office.
313-826-2381


